Healthcare is evolving towards a value-based model where different stakeholder groups in the healthcare ecosystem aim to benefit by partnering to uncover additional value. These value-based partnerships (VBPs) deliver broad value to society by improving patient outcomes, reducing the cost of healthcare delivery, and increasing positive outcomes that benefit the system and society. Taking different forms and involving various stakeholders, VBPs target areas in knowledge-sharing, digital transformation, and reimagining healthcare delivery to reduce high-touch hospital engagement, drive technology-enabled optimizations, and simplify the management of complex care needs.
Pharma can drive VBPs by identifying opportunities along the entire patient journey, moving away from the established role of bringing new innovative products to market and focusing mainly on the point of care. Looking forward, VBPs require decision-making based on the relationships and resources needed for partnership. Simple yet critical steps for successful VBPs can bring partners together in a step-change implementation to uncover value with mutual trust and teamwork. In this paper, we have explored value-based healthcare opportunities and collaborative actions that pharma and key stakeholder groups can engage in to uncover additional benefits for all groups involved. Value-based partnerships can hold the answer to unlock benefits in many areas of the healthcare ecosystem, all while keeping the patient at the center.
“Opportunities exist for stakeholders across the healthcare system to forge these VBPs, shifting the focus to creating value for payers, providers, patients, and all parties within the system.”
Value-based healthcare ecosystem
In a world where healthcare expenditure is set to outpace GDP growth, healthcare systems must find ways to increase value for money. However, with the looming shadow of increasing prices, aging populations, and more complex treatment pathways, it is increasingly difficult to find solutions that provide value across the healthcare ecosystem (Figure 1). At the core of this problem is that each stakeholder defines “value” differently. For pharma, the primary value driver has been bringing innovative products to market that can address unmet needs, developing strategies to succeed in competitive landscapes, and generating sufficient revenues to support their business models. With this mindset, the needs of patients and other stakeholders within the healthcare ecosystem have often taken a back seat in terms of priority for pharma. However, pharma is evolving and acknowledges the opportunity to take a broader view of its role within the healthcare ecosystem.
The answer lies in replacing quantity with quality; this means transitioning from a volume-based healthcare model, which places importance on siloed metrics such as the number of doctor visits and medicines administered, to a value-based system that considers positive outcomes for all stakeholders.
There is mounting evidence that volume-based healthcare can lead to sub-optimal care and resource use, as well as incentivizing behaviors that are detrimental to key healthcare outcomes. (1) Conversely, a value-based system can create external societal benefits while preventing waste in the system. (2) Value-based partnerships (VBPs) between stakeholders are the key to driving this transition, which can produce disproportionate benefits, enabling the entire ecosystem to reap the rewards. (3) Simply put, VBPs engage two or more stakeholders to deliver the highest value to the system and society by improving patient outcomes in a way that is not only mutually beneficial but also reduces the burden on the system. (4) This means abandoning the “everyone for themselves” mentality and instead realizing that everyone can be better off by working together.
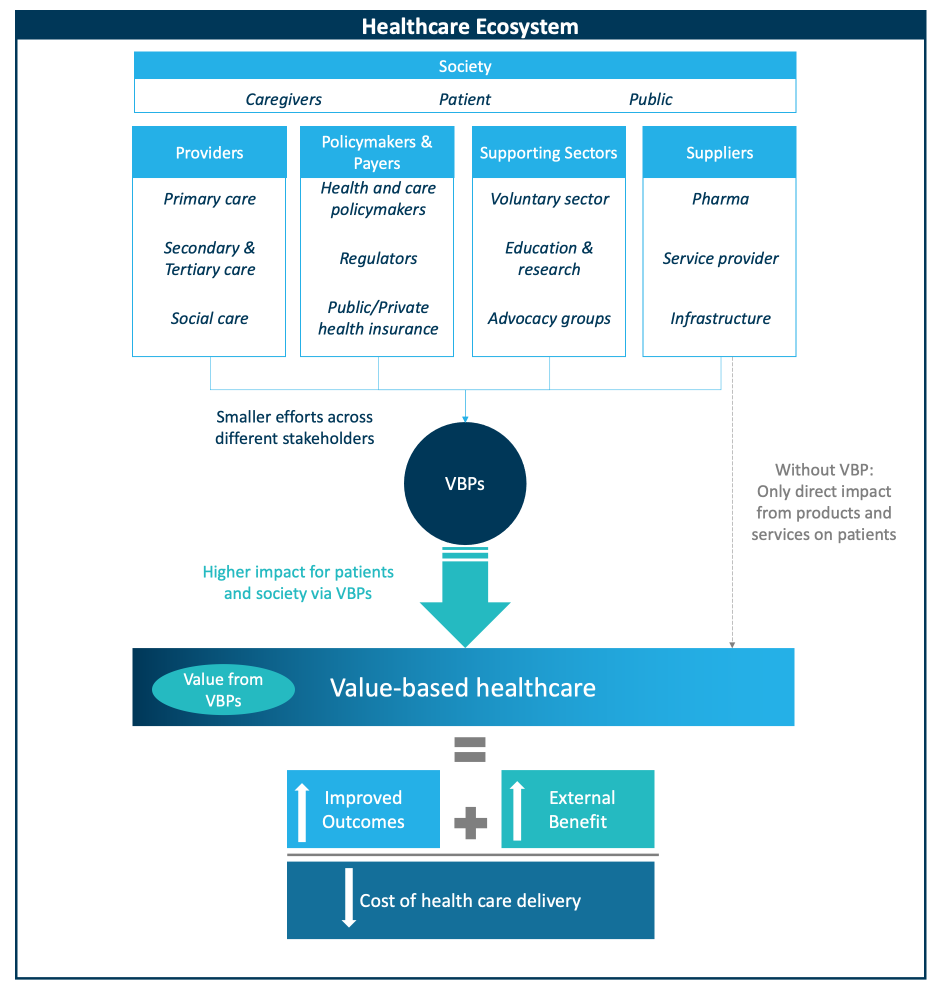
Figure 1. Stakeholders in the healthcare ecosystem; How VBPs can form and lead to increased value in the system
Contrary to popular belief, VBPs can benefit all stakeholders, whether it’s healthcare bodies promoting healthier lifestyles through cost-effective healthcare or pharma providing differentiating wrap-around support for current therapies. To successfully lighten the burden on hospital care, the healthcare system must do more than recognize these types of partnerships; they must actively incentivize their use over the status quo. In the current climate, healthcare systems have also been complacent, looking only at the direct cost of drugs rather than care holistically, which is to the detriment of all other stakeholders, most of all the patient. VBPs can bring forth a multitude of benefits depending on the situation, providing a higher impact on patients and society through the core goal of improving patient outcomes and decreasing societal total costs (Figure 1). It is thus crucial for providers, policymakers, payers, supporting sectors, and suppliers, including pharma, to stimulate value-based approaches and widen the lens to bring societal costs and their impact on the general population into focus. Opportunities exist for stakeholders across the healthcare system to forge these VBPs, shifting the focus to creating value for payers, providers, patients, and all parties within the system.
“When firm foundations are established, the value to stakeholders will be mutually beneficial and collectively positive.“
Value of Partnerships
Partnerships play a crucial role in uncovering value within the healthcare ecosystem; however, to be effective, VBPs must enable each partner to achieve its own goals. From the existing VBP landscape, three key areas are identified: knowledge and expertise sharing, digital transformation, and reimagined healthcare delivery (Figure 2). To derive value in these areas, partnerships must target regions of mutual interest to each stakeholder.
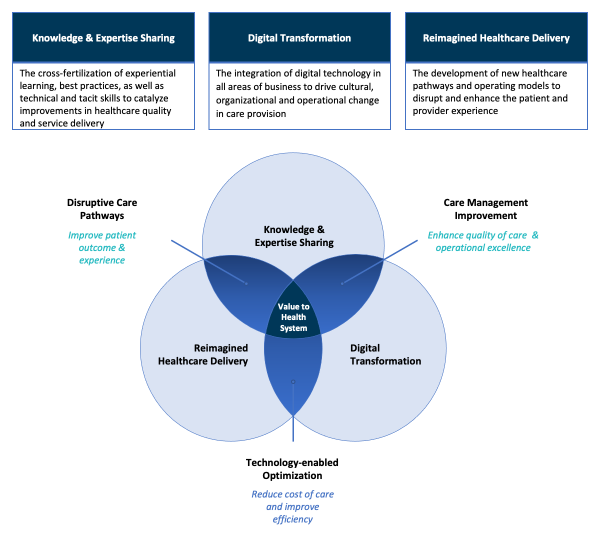
Figure 2. Target areas for stakeholders from the healthcare ecosystem when forming VBPs.
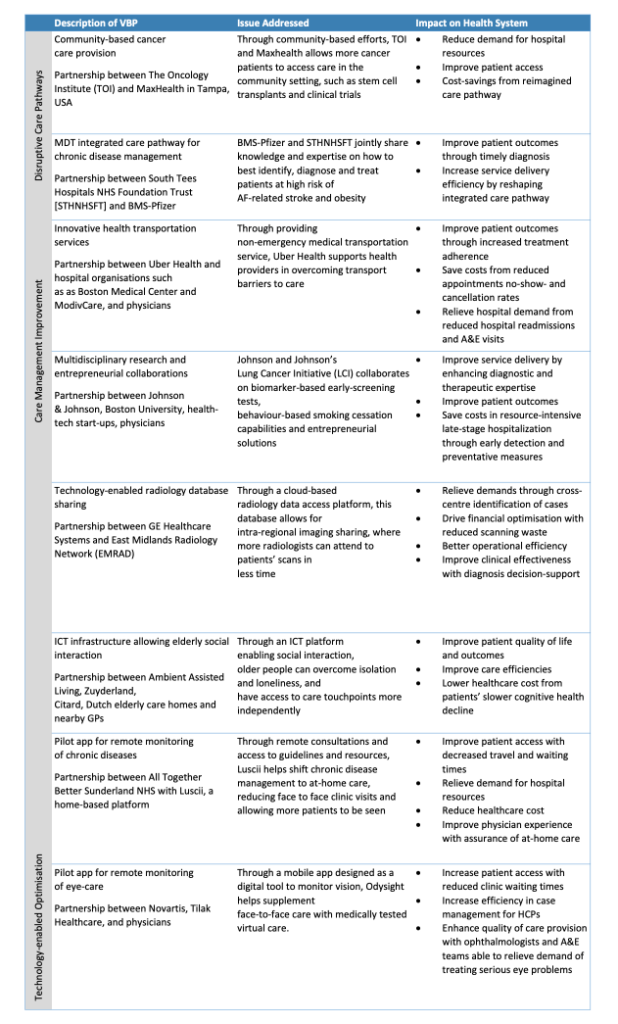
The first area of mutually beneficial value for stakeholders is the disruption of healthcare delivery. Establishing VBPs in this space requires stakeholders to share their expertise and experiential learning, which catalyzes the development of new and innovative practices. Though this sounds simple, such engagement can have disproportionate benefits that decrease hospital burdens and improve patient outcomes across the care pathway, especially in multidisciplinary care settings. The management of cancer is a clear example of where these types VBPs can produce a positive impact. Cancer care requires high-touch communication between specialized oncology experts, secondary and tertiary care providers, and laboratories that work together to decide the optimal treatment option for patients. Innovative VBPs providing community-based cancer care, such as TOI and Maxhealth, offer an alternative model (Table 1). Migrating cancer care into the community setting reduces hospital engagement while simultaneously increasing access; in other words, this disrupts the care pathway to the mutual benefit of multiple stakeholders within the healthcare ecosystem. (5) Similar benefits have been seen for chronic disease management. For example, a collaboration between an NHS Trust and a BMS-Pfizer Alliance has been set up to improve patient and provider outcomes in obesity and atrial fibrillation by implementing multidisciplinary teams (MDT). (6)
The second space that VBPs should target is care management, where transformations can be leveraged to enhance the quality of care while streamlining operations. For these types of initiatives, the healthcare system doesn’t need to reinvent the wheel; instead, it can integrate solutions into existing frameworks to augment care and service provision. Overcoming transportation barriers is one area that VBPs, such as Uber Health, a non-emergency medical transport service, have effectively incorporated digital technology into the existing care paradigm. Here, the provision of ridesharing decreased appointment no-show rates and increased treatment adherence, resulting in improved patient outcomes. (7) In the long-term, this can reduce hospital readmissions and A&E visits, with downstream cost-savings to health providers. (8) Larger scale programs such as JNJ’s Lung Cancer Initiative have forged collaborations that unite academia and entrepreneurial innovation to enhance diagnostic and therapeutic technologies, facilitating advancements in care quality. (9)
Technology-enabled optimization is the third and most active focus of VBPs. The utilization of digital technology enables stakeholders to reimagine how healthcare is delivered, which uncovers value in the form of cost reduction and improved efficiency. Properly executed, digitally enabled processes can revolutionize the patient care journey by opening novel channels of stakeholder interaction. This can be illustrated by partnerships capitalizing on the push for the integration of telehealth and electronic health records, where VBPs can optimize service delivery and care quality via tech-based solutions. VBPs centered around technology can assure an effective continuity of care with a reduced reliance on available resources, primarily through relieving hospital demands, increasing operational efficiencies, and improving patient access to a resulting enhanced quality of care. (10), (11) & (12)
Table 1: Examples of VBPs
Positive externalities can arise from the ripple effect of the impact of VBPs, benefiting the system and society as a whole. VBPs may take different forms and cover diverse opportunities across knowledge-sharing, digitalization, and process optimization. When firm foundations are established, the value to stakeholders will be mutually beneficial and collectively positive.
“Partnerships will be built on the synergistic foundations of expertise sharing, digital transformation, and reimagining healthcare delivery, but trust and teamwork along the journey are required to unlock value.“
Pharma’s Critical Steps for Successful VBPs
Pharma is undoubtedly an integral partner within the healthcare ecosystem; however, it can play a role beyond its contributions to product innovation and take an active hand in uncovering value within the healthcare system to initiate a step change implementation (Figure 3).
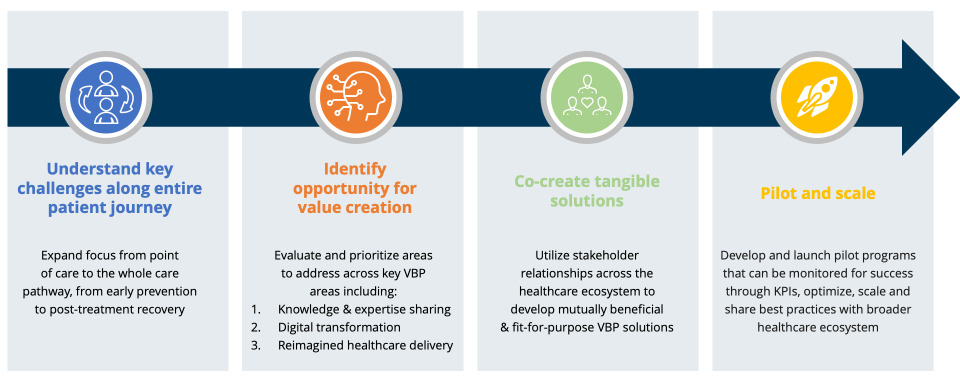
Figure 3: Stepwise process on how pharma can collaborate with other health ecosystem stakeholders to achieve successful VBPs
To drive VBPs, pharma should begin by developing a holistic understanding of key challenges within the therapy areas of interest, examining the care pathway from the perspective of other key stakeholders, such as healthcare providers and patients. Pharma must look before and after treatment and beyond traditional hospital care management. In practice, this involves mapping the pain points of healthcare along the entire patient journey to each stakeholder in the healthcare ecosystem, including in earlier phases of health promotion and prevention, out-of-hospital early assessments, and post-treatment recovery support. This process crystallizes issues and obstacles in the patient experience or healthcare delivery process.
Once these pain points have been identified, pharma can then play an active role in developing solutions. Just as VBPs can target these areas, pain points can be effectively handled by focusing on expertise sharing, digitalization, and improved healthcare delivery (Figure 2). To evaluate and prioritize which areas to play in for maximum impact, pharma needs to view each through the lens of other stakeholders to identify where others would benefit. For providers, this may mean looking at higher patient satisfaction rates and better care efficiencies; for policymakers and payers, more robust cost controls and reduced healthcare spending; for supporting sectors and broader society, advancing disease awareness and knowledge sharing, and better socioeconomic outcomes. Once pharma has clarified value to each stakeholder in the ecosystem, they are well positioned to engage the partners that produce synergistic value across healthcare.
Following this strategic analysis of the playing field, targeted and tangible solutions can be developed to uncover opportunities for health system improvement. First, however, pharma must understand their potential partners’ current requirements and future objectives for the solution to be fit for purpose. Then, to elucidate other stakeholders’ goals and focus on the optimal partnership, pharma should ask a series of questions: what are the underpinning processes, infrastructures, and workforce around the issue? Which stakeholders have a mutual vested interest in solving the problem? How can a problem-solving case be built in tandem with the key stakeholders?
Once the partners have been identified, pharma must be willing to take the journey together; they should empower the other stakeholders to cocreate solutions, maintaining open communication channels to utilize their respective expertise and resources. For every stakeholder to win, they must have an equal voice at the table. Following iterative ideation, pilot programs can be set up, scaled, and monitored for progress. With a robust and collectively crafted project plan, pharma can co-drive the delivery of these programs with partners. Continual impact assessment, stakeholder engagement, and program improvement should be in place to optimize the results of the VBPs while ensuring that each partner continues to benefit. As the partnerships advance toward maturity, program maintenance and enhancement require consistent tracking of relevant KPIs and markers for success. Sharing best practices with the broader healthcare ecosystem will deepen trust and provide a template for further initiatives to be developed.
“For pharma companies, embracing collaborations can elevate their position as significant players within the ecosystem.”
Uncovering Value in Healthcare Together
For value to be realized from dedicated partnerships, stakeholders within healthcare must embrace a new definition of value across the ecosystem. A broader view of value encompasses positive externalities and societal benefits, such as productivity, impact on informal caregivers, and equitable access to healthcare. Healthcare bodies need to recognize that not all VBPs will produce cost-savings in the short term but will arise from long-term efficiencies with resource optimization. Pharma can catalyze value discovery by engaging with different parts of the healthcare system, with a keen focus on the collaborative effort required to capture overall societal value. Together, all stakeholders within the healthcare ecosystem will stand to gain benefits from reimagined value-creation opportunities.
Partnerships will be built on the synergistic foundations of expertise sharing, digital transformation, and reimagining healthcare delivery, but trust and teamwork along the journey are required to unlock value. Being part of an integrated cross-stakeholder delivery team means aligning on the best outcomes and experiences for other players in the system. For pharma companies, embracing collaborations can elevate their position as significant players within the ecosystem. From improving knowledge of patient needs to strengthening relationships with healthcare providers, pharma should welcome the opportunity to play an expanding role within the healthcare ecosystem. With collaboration, VBPs can unlock benefits across all stakeholders in the healthcare ecosystem and ensure the patient is at the center.


